[Warning: Some material may not be suitable for delicate constitutions.]
September 11, 1974
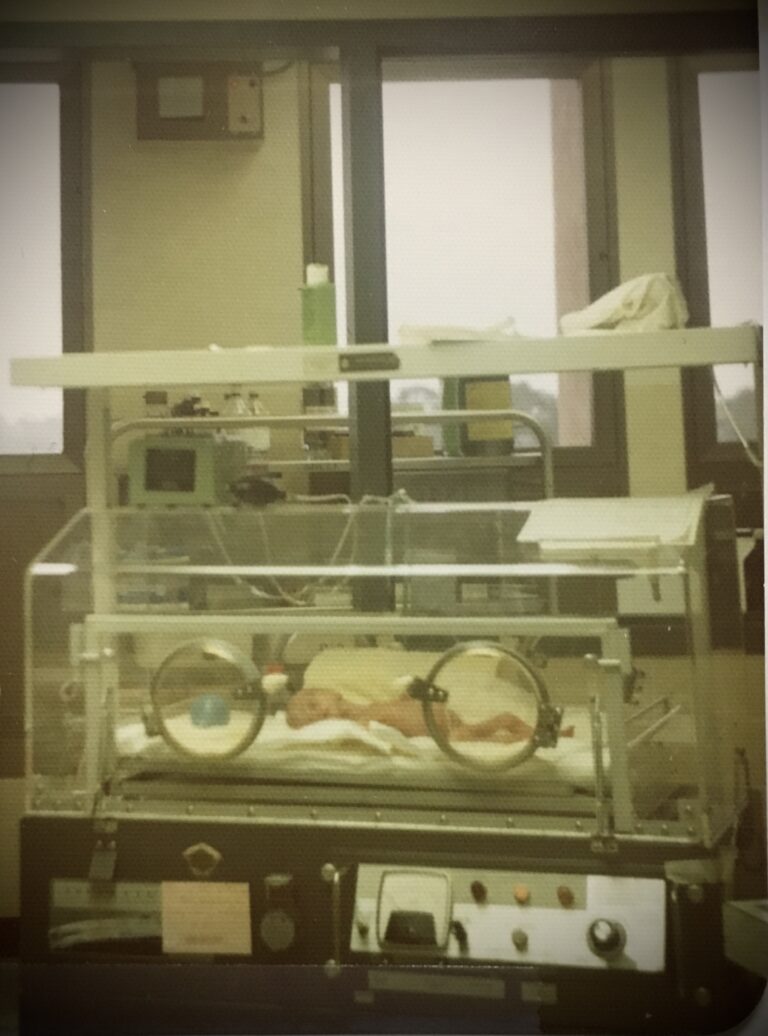
My husband and I stood at the nursery window and stared at the incubator on the other side of the room. Our new baby was lying on a flattened diaper – a preemie diaper that was too large to fasten around her tiny body. The skin stretched so thinly over her closed eyes that she looked like a baby bird. She was frighteningly small.
We weren’t allowed to hold her in the beginning, and even the nurses kept their handling of her to a minimum. She was simply too fragile. All we could do was stand at that window and gaze at her inside the plastic capsule that would be her home for who knew how long. We’d watch the nurses work around her, adjusting things and checking vitals. They would periodically turn her from her stomach to her back and move her head from one side to the other. When they did that, the top of her little ear would sometimes be folded down from where she’d been lying on it. Her dad always panicked when that happened because he was afraid it would stay that way. He’d tap on the window to get the nurse’s attention and motion for her to smooth our daughter’s ear back into place. And the nurse would always comply. My guess is we weren’t the first parents to obsess over their preemie’s condition…even if it was something as trivial as bent ear cartilage.
The events that led us to that place were swift and unexpected. I was six months pregnant and had experienced no physical trauma or unusual health issues. I simply woke up during the night, went to the bathroom and began bleeding profusely.
We’d moved to a new state the week before and I didn’t yet have a doctor. My husband was in the military, so he rushed me to the hospital on base. Prior to this, my only experience as a hospital patient was when I had our first child, and that was at a military hospital in our home state. Everyone I interacted with during my time there treated me with great care and respect. When we arrived at the emergency room at this hospital, I expected the same type of treatment. I soon discovered that those expectations were much too high.
To say I received less than stellar care would be an understatement. While I have no recollection of the person who checked me in, I do remember that when it came to most of the orderlies and nurses, I felt like I was imposing on their time. It’s not that they were blatantly rude – with the exception of the obstetrician – but there was a general air of detachment. I was clearly worried about the state of my pregnancy, yet no one made any effort to ease my fears.
The initial assumption was that I was experiencing placenta previa, a condition where the placenta covers the opening of the cervix, but an ultrasound showed no evidence of that. After running a couple of other tests, they still didn’t have any answers, but they told me I was free to go. I sat up on the examining table and began gushing blood again, so the ER doc said I should probably stay a bit longer for further observation. Had I been as snarky then as I am now, I undoubtedly would have deadpanned, “Good call.”
They kept me lying flat and the bleeding lessened, but I continued to pass large clots. A nurse would closely examine those and when I finally gathered the courage to ask what she was looking for, she matter-of-factly said, “Fetal tissue.” I didn’t know how to respond to that, so I just kept my horror to myself.
Before they had a chance to try and ship me off again, I began having contractions. In an effort to stop them, they hooked me up to an alcohol IV. I don’t know how long I was on that drip, but I do remember hearing a woman in another room screaming with labor pains. An orderly came in to see how I was feeling, and I drunkenly told him I felt great. I then happily suggested they give the woman down the hall the same thing I was getting. I have to confess…that alcohol drip was the highlight of my time as a patient there.
That course of treatment was only temporary, and the contractions started up again the next day. When a nurse came by to check on me, I told her I was in labor and she pooh-poohed the idea, saying it was nothing more than Braxton Hicks. I told her I’d already had one baby and knew labor pains when I felt them. She continued to ignore the situation until it became obvious that the contractions were more severe and much too frequent to be anything but active labor.
It didn’t last long, though. As a matter of fact, I didn’t even make it from the gurney to the delivery table. When the orderlies started to lift me, I made them stop. And when they asked why, I clenched my teeth and said, “I’m having the baby.”
They looked under the sheet and, sure enough, there she was. Of course, at the time, I didn’t know whether I’d had a girl or a boy. I didn’t find that out until after I was transferred to the delivery table for the removal of the afterbirth. And I wouldn’t have known it then had I not made a point of asking one of the nurses. All I got in return was a perfunctory, “Oh, it’s a girl,” as they whisked her away. I remember lying there after that, feeling cold and alone and very, very scared.
A few days later, I was standing at the nursery window when a man came up beside me to admire his own newborn. He pointed his baby out to me and asked about mine. I told him how early she was, that she weighed less than 2.5 pounds when she was born and that I had no idea how long she’d have to remain in the hospital. I also told him I hadn’t been allowed to feed her yet because she was too weak to nurse and had to be given formula through a tube. I was taken aback when he asked if I was planning to breastfeed her once she was able. Right after her birth, a nurse gave me a shot to dry up my milk. I told him this, and he sadly shook his head saying I could have expressed the milk myself until she was stronger. I remember looking away, embarrassed by my own ignorance. They never discussed options with me, and they certainly didn’t ask permission to give me the shot. They just did it. I would have liked to have breastfed her, but I never had the chance.
A uterine infection kept me in the hospital for a week. The day I was released, instead of nestling a baby to my heart, I went home empty-handed.
Within 48 hours, I was back in the emergency room with itchy welts from the top of my head to the soles of my feet. The doctor attributed it to the penicillin I’d received and said I wasn’t to take it again in any form. I told him I’d never before had an allergic reaction to this drug, and I suggested perhaps the breakout was due to nerves. It had, after all, been a very stressful week. My baby was premature, I still hadn’t had a chance to hold her and, while I was still on the delivery table, the stern obstetrician had brusquely informed me my daughter’s chances of survival were slim to none.
The ER doctor either didn’t hear or didn’t care. He simply prescribed an alternate antibiotic and sent me on my way.
The obstetrician told us our daughter’s early birth was due to placental abruption, but he didn’t bother to explain what that meant. After I got home from the hospital, I looked it up in my trusty instruction manual…pretty sure the book was Dr. Spock’s Baby and Child Care. The condition was described as the placenta tearing away from the inside of the uterus and it sounded brutal. The book also said this occurred most often in women over 40 who had experienced four or more pregnancies. This was just my second and I was only 19.
Our other daughter couldn’t understand why her little sister didn’t come home from the hospital with me. She’d been excited to meet her brand new, homegrown playmate and wasn’t the least bit happy with the fact that there was still no baby in the bassinet.
Neither was I. But I wasn’t quite ready to deal with having our tiny girl home yet. I agonized over all the things that could go wrong. And there was one particularly irrational fear that always wrestled its way to the forefront. What if, when we brought the baby home, her sister decided she didn’t want her after all? What if she snuck her into the bathroom and flushed her down the toilet? I examined the opening in the bottom of the bowl and convinced myself her little body would fit. My husband found the whole thing comical and, looking back, I have it admit it was pretty funny. But at the time, the very idea terrified me.
The people working in the neonatal intensive care unit were the polar opposite of those I’d experienced in the OB ward. The level of care I received was subpar at best, but the treatment our baby received was phenomenal. The NICU staff was friendly, attentive and compassionate. And because she really did resemble a baby bird, they lovingly nicknamed our daughter “Tweety.”
Shortly after I was released, we were cleared to go into the nursery to be closer to our baby and we visited every day. We had to gown up, put on surgical masks and scrub to our elbows with soaped pads that felt like sandpaper. It was a cumbersome affair, but it was always worth it.
When I finally held our daughter for the first time, I was unprepared for how weightless she was…and how perfect. A baby boy slept in another incubator nearby, and he had tubes and monitor wires connected all over his body. Our little one had arrived three months too soon and her doctor was cautiously optimistic, but that little guy was full term, and his prognosis was grim. No one could have predicted such a thing, and my heart broke for his parents when he passed not long after.
Our phone rang a few weeks later and, as soon as the caller identified herself as one of the NICU nurses, I felt my knees start to buckle. I was sure she was calling to say they had done all they could but that my baby was just too tiny and weak. I was convinced we had lost our little girl. But that wasn’t what the nurse said at all. Instead, she dragged me from my morbid reverie by telling me they had just removed our daughter from the “Serious” list, and she was improving rapidly. We should be able to bring her home in a few weeks.
For just an instant, anger choked my relief. I visited every day. If the nurse had waited until I arrived at the hospital that afternoon, she could have given me the good news in person. By then my eyes would have already witnessed that my daughter was still alive. Still breathing. Still here. But, instead, I nearly drowned in those few seconds of fear. It took a moment before I managed to appreciate what the nurse was actually telling me, and then all I could do was thank her over and over.
November 11, 1974
Exactly two months after her birth – and one month before she was even due to enter this world – little Jennifer Rae came home.
She did so well in the hospital that, instead of waiting until she reached the usual 5-lb weight requirement, they released her at only 4 ½ lbs. All the newborn clothes we had were still too big, so I made a doll-sized dress for her to wear on Thanksgiving. And we definitely had much to be thankful for. The care she received in the NICU was outstanding. She battled valiantly to survive. And her big sister did not flush her down the toilet.
Miracle of miracles…she lived.
I can certainly remember that time. Even for family members who were far removed from the issue the time seemed to stand still not hearing a word about Jennifer as well as your condition! God certainly had plans for this little girl! Thanks for the rest of the story!
You’re welcome! Just call me Paul Harvey. 😆
Thanks, mom!
I had forgotten about your fear of Jacki flushing me so that was comical to read. 🤣
I’m just grateful she never even tried! 😅
Tears….
♥️
The strength required of preemie parents is unfathomable to me. Your strength is amazing, and has seen you through several crises, I am sure.
And, my I say, you chose a beautiful middle name for your daughter.
Thanks, Pam. ♥️
Just beautifully written Virginia !! I marvel at your strength! Hugs & happy you are so strong Jennifer!
Thanks! 😘
Love this story! Happy birthday, Jennifer!
♥️
Your words painted such a clear picture. Thank you for sharing this personal and emotional story.
Although it ended well (Happy Birthday Jennifer!) it would be so satisfying to strangle the thoughtless, uncaring, and clueless staff who made an already frightening experience worse!
I remember when she was 4 and still small she ate 4 big pieces of Texas chocolate sheet cake and then her meal. Where it went, I had no idea, but we loved it.
Great true story. Thanks, Virginia!
What an ordeal you and Jennifer went through together. So glad that God gave you the strength to handle the events and Jennifer the strength to survive!!
We are nothing if not resilient! Haha!
I read both stories about Jacki and Jennifer.. I had forgotten that Jennifer was born so early. Probably because I had just entered college at IU in late August and I was pretty overwhelmed with the newness of college and living on my own. I am so relieved that she was a fighter and you know that your Mom and my Mom were praying like warriors for her and for you!! You have to beautiful and wonderful daughters. Thank you for sharing Cuz!!
♥️
Did not realize Jennifer was so early. Amazing (and frightening) account.
Do you ever wonder that, if doctors and medical staff were that “unaware” or clueless in the 70’s, how much worse it must have been for mothers just a few decades earlier?
Yes. I imagine a lot of preemies didn’t make it. We were extremely lucky.